Avoid It, Recognize It, Manage It
By Cheri Valle
My Gracie had an esophageal stricture, and it nearly killed her. She developed it from her medications. Here is PetMD’s definition of esophageal stricture: “The esophagus is the tubular organ that runs from the throat to the stomach; an esophageal stricture is an abnormal narrowing of the internal open space of the esophagus.” Esophagitis is an inflammation of the esophagus, hopefully short term but which could progress to a stricture. Either esophagitis or esophageal stricture is a serious problem that can make it difficult for your cat to eat or even breathe.
The PetMD article goes on to list causes of esophageal stricture. Those relevant to our kitties include:
Esophageal retention of pills and capsules
Persistent vomiting
Backward or reverse flow of stomach contents into the esophagus, unrelated to anesthesia (gastroesophageal reflux disease).
Pretty much every IBD kitty is at risk, because so many need daily, long term meds. And many of us have cats with chronic vomiting; a few IBD kitties have reflux. Each of us needs to know about the dangers and how to avoid them. Each of us needs to know what esophageal stricture looks like (no, it’s NOT a hairball!) in order to get the kitty to the vet sooner rather than later. And if it happens, each of us needs to know that it can be managed… but only if you know what to do.
AVOIDING ESOPHAGITIS AND ESOPHAGEAL STRICTURE
This is obvious – prevention is the best cure! Let’s take each cause, one at a time. If your cat is vomiting repeatedly or has reflux, you need to get it under control. That’s a vet issue – you and your vet need to determine in your cat’s particular case how to address the problem. But the key point is: it can’t be ignored.
Administering pills and capsules is probably the most common way our cats might get esophagitis, which can lead to actual esophageal stricture. Here is the key point: you MUST make sure every single pill or capsule is cleared out of your cat’s throat. You can’t skip even one time. Cats’ anatomy is such that they simply don’t clear pills out of their throats on their own with “dry” pilling, and so they are especially prone to damage caused by pills. This article cites a study about the dangers of dry pilling, http://catinfo.org/pilling-cats-and-dogs-and-erosive-esophagitis-compounded-flavored-liquid-alternatives-transdermal-medications-pill-pockets/.
Cats were tested to determine how long it takes for pills without a “chaser” to clear out of the throat. Here is what it said: “After 5 minutes 84% of capsules and 64% of tablets are still sitting in the esophagus.” [It is important to note that gelcaps are even worse than tablets in clearing out of the throat.] Certain categories of medications, including antibiotics, can cause the most damage if they aren’t cleared out of the esophagus. There are case studies in veterinary research websites about cats that have died from a single dose of certain medications such as clindamycin or metronidazole. And how many of our kitties are prescribed antibiotics such metronidazole at some point? Here is a summary of the article: If you can get your cat to voluntarily drink something liquid like bone broth or eat something semi-liquid like canned food pureed with a lot of water, use that. If your cat will tolerate syringed water after pilling, use that – see the pilling instructions https://www.ibdkitties.net/how-to-pill/. If the best you can do is to get your cat to eat his regular food or even a cat treat afterwards, do that. The point is, do something!!!
One of the ways many vets try to avoid the dangers of esophagitis and esophageal stricture is to prescribe liquid medications. The vets might think, as my local vet did, that they have avoided the dangers of pilling and the problem is solved — no need to clear liquids out of the throat. This is not true! You must follow the same instructions for clearing meds if you are using compounded liquids. Liquids are in fact safer – you can’t kill your cat with a single dose if you fail to follow the clearing instructions – but your cat can develop esophagitis and esophageal stricture from liquid meds. Gracie did. The vets from the Colorado State University Veterinary Teaching Hospital (CSU VTH) have done a lot of research on this subject. By chance, that is where my local vet referred us when Gracie started having trouble. Our wonderful internal medicine vet there gave me a long lecture about clearing liquid meds. When I got back home, I repeated this all to my local vet, wondering why she had never told me about it – and she said she just plain didn’t know. Gracie lived with the consequences of mine and my local vet’s ignorance for a long time.
GRACIE’S STORY
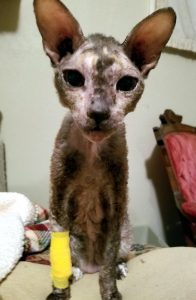 Gracie was a really complex cat. She had IBD and pancreatitis which were mostly stable but periodically gave her trouble. She also had nasal lymphoma, CKD, stomatitis, heart disease, prednisolone-induced diabetes. I’ve probably forgotten a few other things. At the time she developed her esophageal stricture she was about 10-1/2 years old and it was maybe six weeks after she was diagnosed with nasal lymphoma. Her cancer is another story that won’t be told here. (Short form: she received one stereotactic radiation treatment at CSU VTH and 14 months later was doing reasonably well other than a persistent URI.) But the key issue is she was on a lot of twice-daily pills and capsules: tylosin, cisipride, prednisolone. I’ve been pilling cats for 30 years and I ALWAYS use a chaser of some kind. Gracie was good about a syringed water chaser (unlike a few other cats I could mention!) and so I used that method with her. One day about 6 weeks after her cancer diagnosis, she choked on a pill. As soon as she stopped choking I immediately chased the pill with about 9 cc’s of water. At the same time, she was on liquid doxycycline for her persistent URI. The doxy sometimes makes her throw up, so I was very carefully giving it last thing at night just before she went to sleep, after her late-night meal. At the time I didn’t know I had to chase liquids with water also, so I would give that liquid doxy and it would sit un-cleared in her throat all night long.
Gracie was a really complex cat. She had IBD and pancreatitis which were mostly stable but periodically gave her trouble. She also had nasal lymphoma, CKD, stomatitis, heart disease, prednisolone-induced diabetes. I’ve probably forgotten a few other things. At the time she developed her esophageal stricture she was about 10-1/2 years old and it was maybe six weeks after she was diagnosed with nasal lymphoma. Her cancer is another story that won’t be told here. (Short form: she received one stereotactic radiation treatment at CSU VTH and 14 months later was doing reasonably well other than a persistent URI.) But the key issue is she was on a lot of twice-daily pills and capsules: tylosin, cisipride, prednisolone. I’ve been pilling cats for 30 years and I ALWAYS use a chaser of some kind. Gracie was good about a syringed water chaser (unlike a few other cats I could mention!) and so I used that method with her. One day about 6 weeks after her cancer diagnosis, she choked on a pill. As soon as she stopped choking I immediately chased the pill with about 9 cc’s of water. At the same time, she was on liquid doxycycline for her persistent URI. The doxy sometimes makes her throw up, so I was very carefully giving it last thing at night just before she went to sleep, after her late-night meal. At the time I didn’t know I had to chase liquids with water also, so I would give that liquid doxy and it would sit un-cleared in her throat all night long.
About two weeks after that pill-choking incident, she started having a lot of trouble eating. Each time she began eating, she would go into five minutes of coughing, neck stretched out, with some lip-licking and head-bobbing and generally nasty noises. It looked kind of like a cat trying to get rid of a hairball – but Gracie is a semi-bald Cornish Rex and she’s never had a hairball in her life. And it happened around eating (or pilling). My local vet immediately referred us to CSU VTH. Yippee, another road trip. Gracie’s internal medicine vet, whom I dearly love, did an endoscopy procedure for diagnosis. She told me that Gracie had an esophageal stricture. In Gracie’s case, her stricture was more like a long area of inflammation rather than a single tight point. It was located close to the top of her esophagus, which meant that if food backed up in there she would quickly reach the point where it is blocking her windpipe. The vet also told me that Gracie probably got her stricture from the two weeks of liquid doxycycline. The pill-choking incident may have contributed, but wasn’t the major cause. This is when I learned that for many years and many cats, I have been hurting my cats by not clearing liquid meds from their throats.
The treatment: (including bumping up Gracie’s prednisolone), which at the time we had been trying to taper. We tried her on sucalfrate “slurry” which was a dismal failure because she hated it so much I couldn’t administer it. She also was never again in her life given any pill or capsule (more about how to avoid this later). We dropped two of her meds – tylosin and cisipride – simply because they were capsules. And her diet was changed to semi-liquid pureed food (more about this later too).
 A couple of months after that, Gracie clearly was going downhill. She was hungry and demanded food, but couldn’t eat it. As soon as she began eating, she would start choking. On one particular weekend she tried eating but the food just ran out of the sides of her mouth. I decided this was it, and was spending what I thought was my last weekend with her. But I couldn’t stand it. I took her to a new vet, the only one I could find who would answer the phone, and told the vet to either help her or euthanize her. The vet recommended euthanasia, but agreed to try to open Gracie’s throat surgically. It was a wild and crazy procedure that the vet made up on the fly, using the kind of narrow tube that vets use to dislodge blockages in a male cat’s penis. I watched as they put Gracie under using gas only (remember she has heart disease – she’s a high risk anesthesia candidate) and ran the tube down her throat. We had been trying to taper Gracie’s pred, which in retrospect was a big mistake, so the vet bumped it back up to a high dose.
A couple of months after that, Gracie clearly was going downhill. She was hungry and demanded food, but couldn’t eat it. As soon as she began eating, she would start choking. On one particular weekend she tried eating but the food just ran out of the sides of her mouth. I decided this was it, and was spending what I thought was my last weekend with her. But I couldn’t stand it. I took her to a new vet, the only one I could find who would answer the phone, and told the vet to either help her or euthanize her. The vet recommended euthanasia, but agreed to try to open Gracie’s throat surgically. It was a wild and crazy procedure that the vet made up on the fly, using the kind of narrow tube that vets use to dislodge blockages in a male cat’s penis. I watched as they put Gracie under using gas only (remember she has heart disease – she’s a high risk anesthesia candidate) and ran the tube down her throat. We had been trying to taper Gracie’s pred, which in retrospect was a big mistake, so the vet bumped it back up to a high dose.
And it worked! Gracie was able to eat a little. With the help of some transdermal mirtazapine (appetite stimulant), she was back to eating a lot. At times her esophageal stricture would worsen for a while, which I addressed by bumping her pred short term and making her food even more runny. She did develop diabetes from all that pred, but I switched her to a very low carb diet and she no longer needed insulin. Because of her cancer, every day I had with her was a gift.
UPDATE July 2017: Gracie died in May as the cancer did come back; I expected that it would. I made the decision not to pursue another round of cancer treatment, due to all her other health issues at the time. She was tired, and ready to rest. My Gracie, my love, is gone…. But I can only hope her story will help others.
RECOGNIZING ESOPHAGITIS AND ESOPHAGEAL STRICTURE
This definitely is a problem that must be diagnosed by a vet. There are other issues that can look much the same. Asthma, pneumonia, heart disease, tracheitis (inflammation of the trachea), rhinotraceitis (inflammation of the nose and trachea)… all can cause coughing in cats. Symptoms depend somewhat on how far down the throat the inflammation or stricture is. The closer to the mouth, the more you will see coughing. In some cases your cat won’t cough at all – she will simply refuse to eat.
Here is a list of symptoms from the PetMD article:
Regurgitation (return of food or other contents from the esophagus)
Liquid meals are often tolerated better than solid meals
Difficulty swallowing is seen with upper esophageal strictures
Howling, crying, or yelping during swallowing when the cat has active inflammation of the esophagus
Good appetite initially; eventually, lack of appetite with progressive esophageal narrowing and inflammation
Weight loss and malnutrition as the disease progresses
Weight loss to severe weight loss with muscle wasting in cats with chronic or advanced stricture
Excessive production of saliva and drooling, and/or reacting in pain when touched on the neck and esophagus may be seen in cats with inflammation of the esophagus at the same time the stricture is present
Progressive regurgitation and difficulty swallowing may lead to aspiration pneumonia
Abnormal lung or breathing sounds, such as wheezing and coughing, may be detected in cats with aspiration pneumonia
And of course, it could be just a hairball!
Here are the key things to know: If you cat has frequent or prolonged coughing or choking incidents that don’t result in vomiting up a hairball, take him to a vet, especially if these incidents are mostly associated with eating or pilling. If your cat seems to be hungry and not nauseated but refuses to eat, make sure you and your vet consider esophagitis or esophageal stricture as a possibility. Before she began treatment, Gracie’s coughing/choking fits were set off by eating and often lasted about 5 minutes. To repeat: if your cat does this multiple times and does NOT actually vomit, get her to the vet NOW. Diagnosis of esophageal stricture is made by either a barium swallow x-ray, or an endoscopy. There are a lot of good pictures on the internet from cat endoscopies of what it looks like – it’s pretty frightening.
MANAGING ESOPHAGEAL STRICTURE
Esophagitis – inflammation – needs to be treated quickly, and will hopefully heal. Here are the treatment recommendations from a website named Fireside Pharmacy: “Suggested therapy for esophagitis includes sucralfate slurries, a prokinetic agent (i.e. cisapride) to increase lower esophageal sphincter tone, and anti-inflammatory doses of glucocorticoids to prevent stricture formation.”
If the inflammation has progressed to an actual stricture, it may never heal. So you need to be able to manage it long term. Your cat may have complicating factors also, such as aspiration pneumonia. Treatment may need to get immediate issues like this under control, before beginning long term care. If the stricture is a specific tight point, it may be treatable with a surgical procedure using a balloon catheter to open the tight spot. This treatment is often repeated multiple times, either over a few days or periodically over months. In Gracie’s case this procedure wouldn’t have worked, because her stricture was a longer area of inflammation. In extreme cases, the only solution to esophageal stricture is a feeding tube. https://www.ibdkitties.net/feline-esophagostomy-tubes/. Your vet will deal with medical recommendations such as prednisolone and sucalfrate. This article is focused on things you as a pet parent can do.
In a short term situation – your cat just started having a choking/coughing fit and you don’t think it’s one of the other causes such as a hairball, heart disease or asthma:
1) Don’t do anything until well after she stops choking and coughing – this should be obvious. If it’s really prolonged, just get to the vet.
2) If your cat tolerates syringed water and you are REALLY GOOD at doing this, syringe about 6 ml’s of water in very small increments. Remember, cats with esophagitis or esophageal stricture are way more prone to aspiration pneumonia than other cats, so don’t do this unless you are really confident in you and your cat’s ability to avoid aspiration. https://www.ibdkitties.net/syringe-feeding/
3) Offer something yummy and liquid, like chicken broth, bone broth, or (if your cat can tolerate seafood) tuna water. Instructions for tuna water are in the catinfo.org article. Instructions for bone broth and chicken broth are here: https://www.ibdkitties.net/bone-broth/. (Don’t use commercial beef or chicken broth – too much salt.) Fancy Feast Broths work also – just drain the liquid and offer that rather without the solids. I keep Fancy Feast Broths in my house at all times so I have a liquid that cats will go for which doesn’t require any preparation on my part.
4) Puree some canned food with water, at least 1 part water to 2 parts food. If you don’t have a blender or food processor to puree with, just mash some food with water. Hopefully your cat will mostly lick the water off the top.
5) Don’t feed for at least a few hours after a major choking fit. When you do feed, offer the pureed canned food only. Pick up ALL dry food in the house so your cat can’t get to it.
In the long term if your cat has an esophageal stricture, here are some management steps you can take:
1) NO PILL OR CAPSULES EVER, even if chased with water. Try to get your medications compounded into liquid or transdermal form. If this is impossible, for example with certain new and proprietary meds like Cerenia, convert your pills into liquids. Put the pill (broken into pieces if necessary) into a dosing syringe – just pull the plunger out and drop the pill in. Then suck up enough water to dissolve the pill and let it sit for half an hour to an hour, while the pill dissolves, and shake well. This may take some experimentation – some pills must be crushed a bit to do this. Capsules are easier. Suck up the water first and put your finger over the end to hold it while you remove the plunger. Dump the capsule contents into the syringe. Replace the plunger and shake.
2) Use transdermal meds for everything you can.
3) If you can get your cat to eat her meds blended in her food, do that – it’s safer. Be super careful with any syringed liquids (meds, water, food when necessary) to avoid aspiration. Any cat with an esophageal stricture is at high risk for aspiration pneumonia.
4) If you must use liquid meds, religiously chase them with water, food, or something. See the catinfo.org article for suggestions.
5) NO DRY FOOD, EVER. No treats either.
6) Feed only pureed, canned pate style food blended about 2 parts food to 1 part water. The easiest way to puree food is with a hand blender, so there is less waste than you get when you puree something as small as a can of food in a large blender or food processor. I have a Hamilton Beach hand blender that I bought at Walmart for about $22 – it works really well. Gracie ate Fancy Feast Classics. I pureed three cans at a time in a covered container. I also added in her Miralax and potassium gel at the same time, so she never even knows she’s getting it – much easier!
7) Feed many very small meals. Gracie literally ate only a couple of tablespoons at a time, and she ate maybe 8 or 10 times a day, even more sometimes. These don’t have to be spread out evenly during the day. I kept Gracie’s food beside me in the evenings when we are relaxing watching TV, and every time she demanded food I offered it again. To avoid having to get up in the middle of the night, I kept her food next to my bed on top of one of those frozen gelpacks in a plastic dish – instant refrigerator.
At first, esophageal stricture seems impossible to manage. But don’t panic — it can be done! When Gracie was first diagnosed, someone posted about her cat who lived for years with a very tight stricture. Like so many issues with our IBD Kitties, this is not as impossible as it seems.
http://www.petmd.com/cat/conditions/digestive/c_ct_esophageal_stricture
www.ibdkitties.net/bone-broth/
www.ibdkitties.net/syringe-feeding/
